Supporting Technologies
Consumer E-Health and Health Metrics -> FrameworksThe page below discusses three key topics:
E-health
Expansion of health information technology and various e-health tools such as mobile health apps or secure email messaging between patients and providers, have created new opportunities for people to participate more actively in monitoring their health and directing their health care, detailed in an article in Health Affairs. As described in their consumer e-health program, the ONC’s three objectives regarding health information technology (IT) are access, action, and attitudes. These are described in more detail in the following table (drawn from this Consumer e-health program overview):
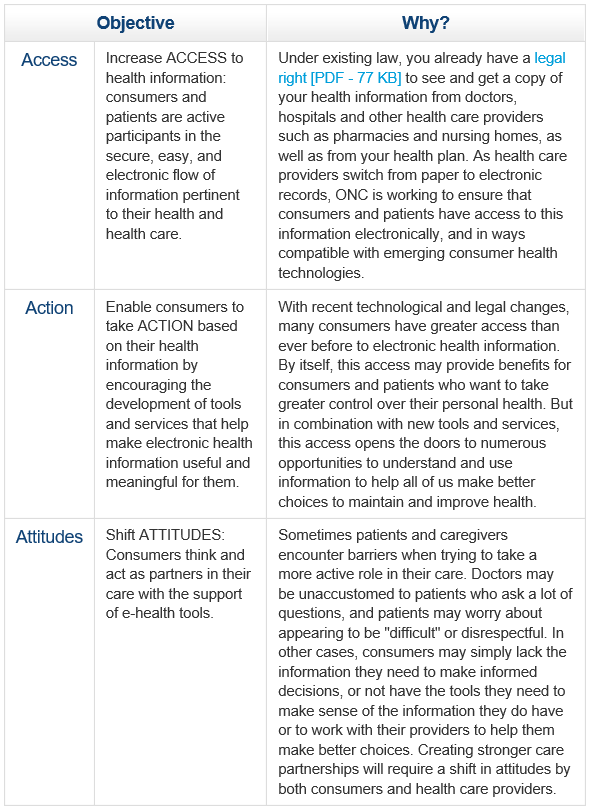
Source: HealthIT.gov. Consumer e-health program overview.
Examples of consumer e-health applications are set out in this helpful article. They include:
- Peer-to-peer online support groups/health-related virtual communities in which individuals who share similar health concerns meet virtually.
- Self-Management/Self-monitoring in which the patient has a central role in managing their illness, or they use a monitoring system of some sort, such as a phone app, fitness tracker, or smartwatch.
- Decision aids that facilitate decision-making through the presentation of information on options and outcomes for an individual’s health condition.
- Personal health records, or electronic tools that allow individuals to track and access their health information.
- Internet use to acquire health information from the World Wide Web.
Antonia Hordern and colleagues (2011) conducted an extensive literature review to assess the evidence of consumer use of e-health applications. The following table provides a comparative summary of different types of e-health applications along with their purposes, strengths and weaknesses.
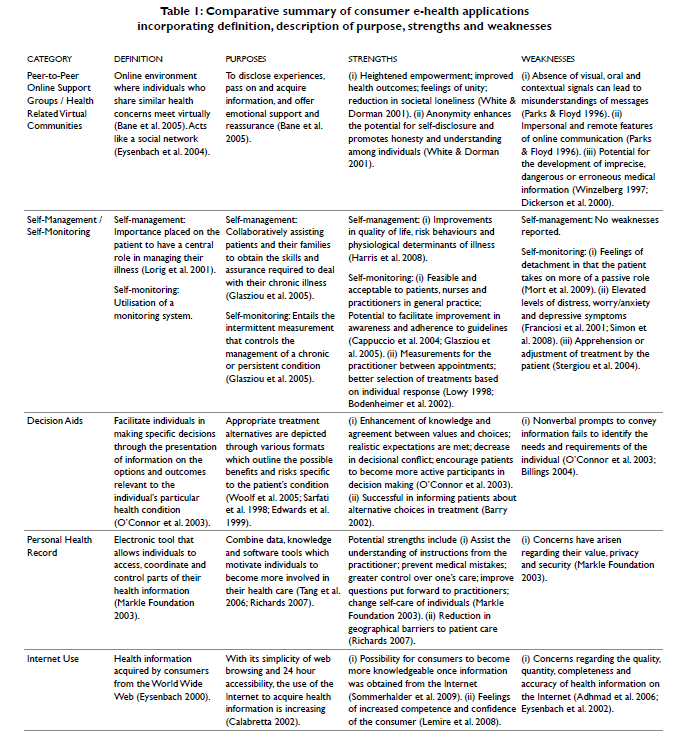
Source: Consumer e-health: an overview of research evidence and implications for future policy. Health Information Management Journal.
Health Metrics
The relationship between individual and population health is built on the distinction between clinical medicine and public health, though it is difficult to talk about one without the other, as described in an article on the relationship between individual and population health. In an environmental scan of integrated approaches, Jacobson and Teutsch suggest considering an integrated measurement framework that includes three areas:
- Population health, including total population health and the health of subpopulations.
- Sample metric: an individual’s cholesterol level (clinician’s concern), or percentage of a population with high cholesterol (public health official’s concern).
- Determinants of health, such as genetics/biology, clinical care, behaviors, and the social and physical environments.
- Sample metric: Exposure to lead.
- Health improvement activities undertaken by the clinical system, public health system, or multi-sectoral collaborations.
- Sample metric: Percentage of people with diabetes who had their hemoglobin A1c measured in the last six months.
Jacobson and Teutsch reviewed over 25 indicator reports and found a common set of health metrics in a variety of categories (see table below.)
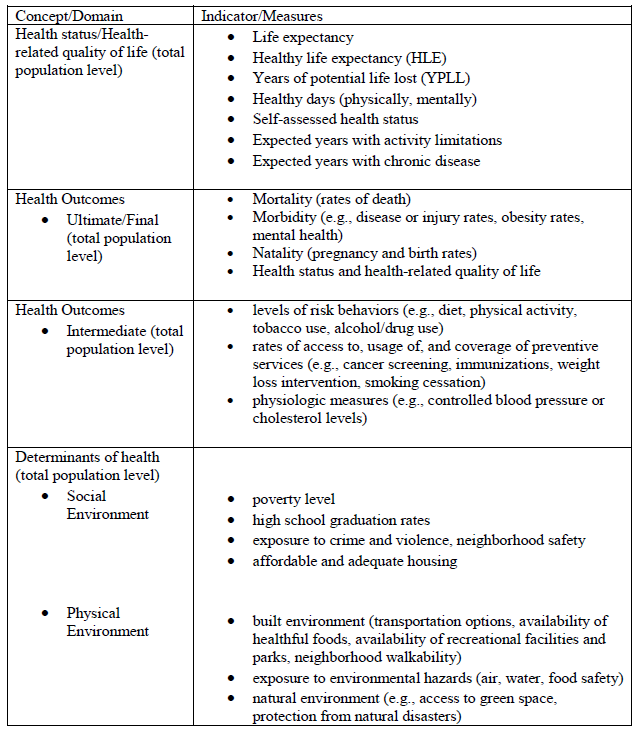
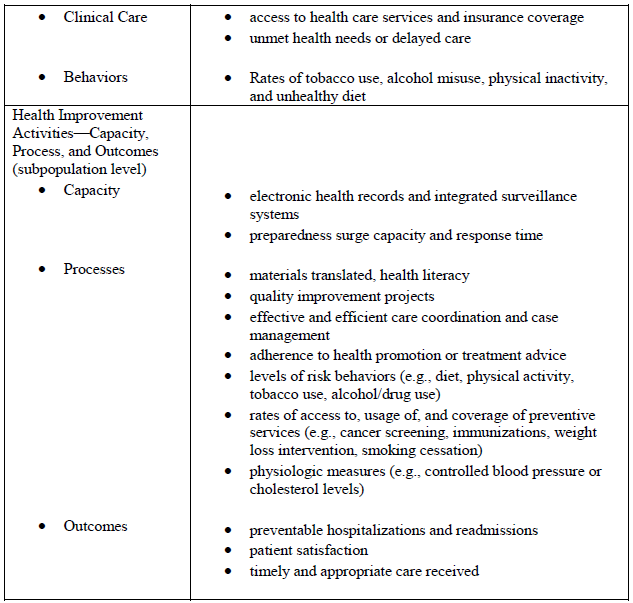
Examples of Metrics used to assess total population health, the determinants of health, and health improvement activities from multiple indicator reports.
Source: Jacobson DM & Teutsch S. (2012). An environmental scan of integrated approaches for defining and measuring total population health by the clinical care system, the government public health system and stakeholder organizations, p. 22.
Patient-Reported Outcomes
Patient-reported outcomes (PROs) are any reports of the status of a patient’s health condition that comes directly from the patient, without interpretation of the response by a clinical provider or anyone else. (See Patient-reported outcomes: A new era in clinical research.)
Although medical technology provides the physiological or biochemical patient data, it does not provide all data about a treatment for disease. Only a patient can describe his or her thoughts, complaints, and opinions.
In PROs, providers go beyond physiological or biological measures and ask patients to describe their:
- physical functions
- symptoms
- global judgments of health
- psychological well being
- social well-being
- cognitive functioning
- role activities
- personal constructs
- satisfaction with care
- health-related quality of life
- adherence to medical regimens
- clinical trial outcomes
PROs serve to empower the patient as they report on how health care is impacting them. The patient information is necessary for determining the efficacy of a treatment, and the dialog helps in building rapport between a patient and his or her healthcare provider.
Data collection using a PRO instrument can be self-administered by answering a survey in writing or on an iPad; or through an interview, whether in person or by telephone or email. Electronic PROs, meaning those that collect data through electronic diaries, computers, or iPads are more beneficial than paper-based PROs because they avoid data entry errors and give immediate access to the data. They also increase a patient’s willingness to share sensitive information. (See Patient-reported outcomes: A new era in clinical research.)
PRO measures (PROMs) refer to various scales, measures, and instruments that enable researchers to assess patient-reported health status for physical, mental and social well-being. (See Patient-reported outcomes (PROs) in performance measurement.)
A PRO-Based performance measure (PRO-PM) is a performance measure that is based on PROM data that is aggregated for a healthcare entity, such as the percentage of patients in an accountable care organization whose nine-item patient health questionnaire (PHQ-9) depression score has improved.
Distinctions among PRO, PROM, and PRO-PM: Two Examples
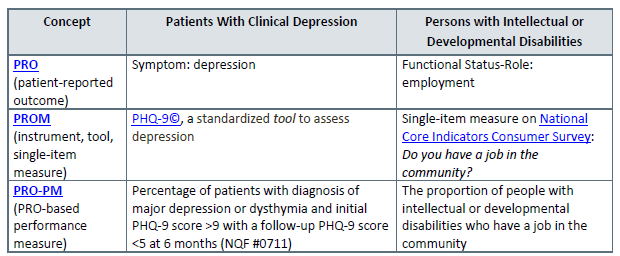
Source: National Quality Forum, 2013
