It Begins with You
Patient Engagement > Patient ActivationPatient Activation
Patients who are more “activated” or more involved in their health tend to have better health outcomes and lower costs than those who are less activated. Findings from over 180 peer-reviewed studies (Hibbard, 2015) indicate that:
- Higher activated individuals are more likely to engage in positive health behaviors and to have better health outcomes.
- Higher activated patients tend to have better care experiences.
- Higher activated patients have lower costs. Hibbard (2015) found that after controlling for demographics and health status, activated patients cost $1,987 less per patient annually than lower activated patients, which is a 31% difference in cost.
Four Stages of Activation
Hibbard et al., (2004) describe four stages of activation. Patients:
- Believe they have an important role in their own health care;

- Develop both the knowledge and confidence needed to take an active role in their care and health management, including an understanding of how to access and use the health care and supportive services available to them;
- Translate this confidence and knowledge into action; and
- Maintain an active role in their health care, even when faced with challenges to doing so.
Tasks that Support Activation
The six core tasks that support activation as identified by Hibbard et al. (2004) are:
- Symptom self-management

- Engagement in actions that support health and functioning maintenance
- Involvement in treatment decision making
- Collaboration with health care providers
- Critical, performance-based selection of providers
- Navigation of the provider system
Patient Activation Measure – Health
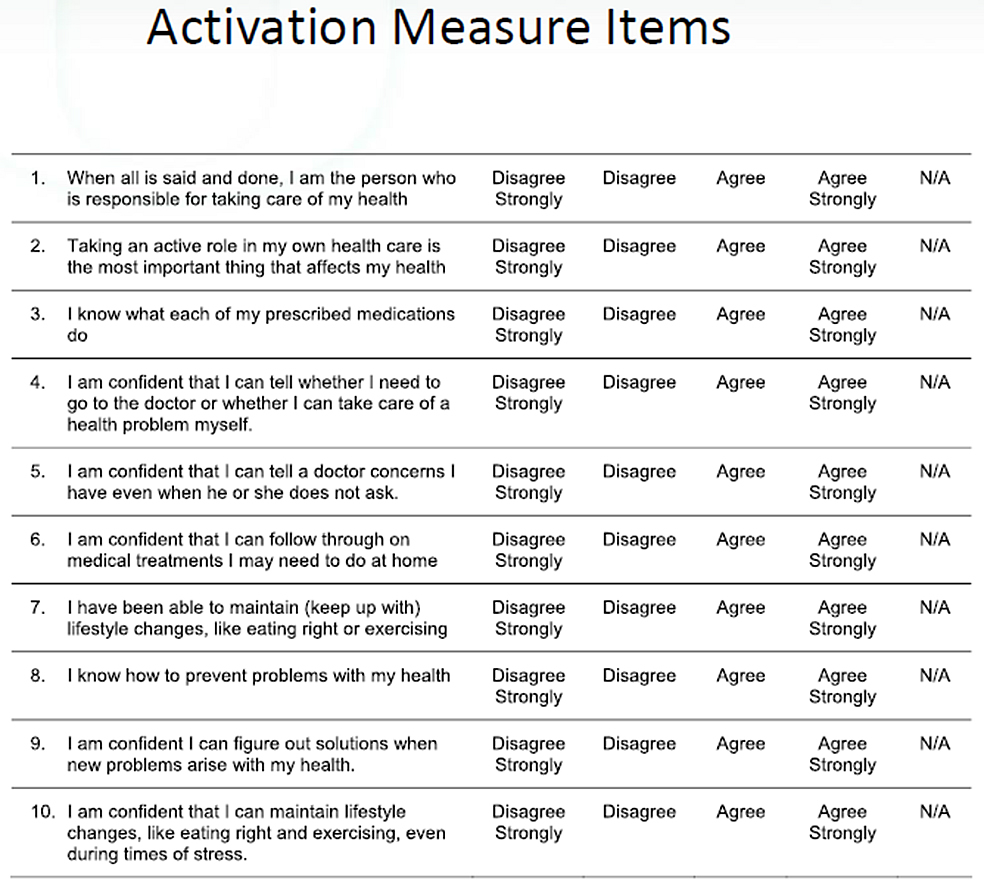
Although there was wide agreement among researchers and health care providers that it was important to engage patients in their own care process, it was not possible at one time to draw conclusions on whether those who were more activated had better health outcomes or lower health care costs. Hibbard (2004) decided to try to develop a tool that would measure patient activation. Ultimately she and her team successfully developed the Patient Activation Measure (PAM). Not only does using it enable researchers to measure health outcomes, but it also gives a provider information on how to customize interventions for their patients. A patient who is less activated in their health may need more information about their condition and treatments. Patients who are more activated may need interventions to increase their skills and confidence. The following figure shows examples of questions that the PAM asks to determine a patient’s activation level.
Source: Hibbard et al. (2004, August). Development of the Patient Activation Measure (PAM): Conceptualizing and Measuring Activation in Patients and Consumers. Health Serv Res. 39(4 Pt 1): 1005–1026.
Patient Activation Measure – Mental Health
A research team led by Carla Green, which included Judith Hibbard, conducted a study to assess whether they could develop a valid and reliable measure of patient activation among individuals with serious mental health problems. The original Patient Activation Measure (PAM) focused on physical conditions and contained items measuring self-assessed knowledge about chronic conditions, beliefs about illness and medical care, and potential for self-care. The new measure, PAM-Mental Health (PAM-MH), adapted the original PAM to assess for mental health-related activation. The revised questions are shown in the figure below.
Source: Green, C. A., Perrin, N. A., Polen, M. R., Leo, M. C., Hibbard, J. H., & Tusler, M. (2010). Development of the Patient Activation Measure for Mental Health (PAM-MH). Administration and Policy in Mental Health, 37(4), 327–333. https://doi.org/10.1007/s10488-009-0239-6
Researchers in this study concluded that the PAM-MH is a valid measure to use with populations with a mental health diagnosis. In comparing respondent scores, they found that those who scored higher on activation also did better on measures of recovery, following directions on psychiatric medication, and having a better quality of life. These findings mirror those of the original PAM.