It Takes a Village
Peer Family and Community Support -> Non-Traditional Health WorkerNon-Traditional Health Worker
The State of Oregon passed landmark legislation in 2011 defining Oregon’s approach to the inclusion of non-traditional health workers in their emerging Coordinated Care Organization health reform structure. This section of the E-Guide draws on this effort, describing the following components of a non-traditional health worker framework:
- Types of Non-Traditional Health Workers
- Roles in the Health Care System
- Funding Streams
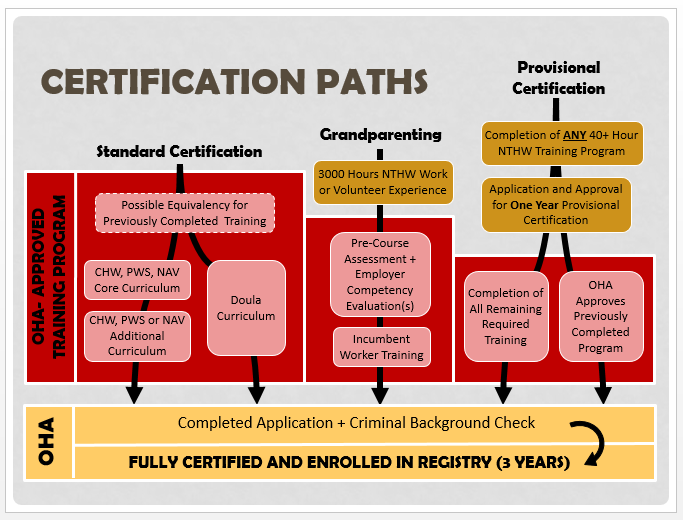
- Certification Paths

Types of Non-Traditional Health Workers
Oregon’s Health Care Workforce Committee has defined four types of non-traditional health workers: Community Health Workers, Peer Wellness Specialists, Personal Health Navigator, and Doulas.
Community Health Worker means an individual who promotes health or nutrition within the community in which the individual resides, by:
- a) Serving as a liaison between communities, individuals and coordinated care organizations;
- b) Providing health or nutrition guidance and social assistance to community residents;
- c) Enhancing community residents’ ability to effectively communicate with health care providers;
- d) Providing culturally and linguistically appropriate health or nutrition education;
- e) Advocating for individual and community health;
- f) Conducting home visitations to monitor health needs and reinforce treatment regimens;
- g) Identifying and resolving issues that create barriers to care for specific individuals;
- h) Providing referral and follow-up services or otherwise coordinating health and social service options; and,
- i) Proactively identifying and enrolling eligible individuals in federal, state, local, private or nonprofit health and human services programs.

Peer Wellness Specialists build on the already existing designation of Peer Support Specialist, which Oregon defines as:
(a) A self-identified person currently or formerly receiving mental health services; or
(b) A self-identified person in recovery from a substance use disorder, who meets the abstinence requirements for recovering staff in alcohol and other drug treatment programs; or
(c) A family member of an individual who is a current or former recipient of addictions or mental health services.
The Peer Wellness Specialist designation expands the role from services focused on behavioral health and addictions recovery to include physical health promotion, and disease prevention and intervention activities for individuals and their families who experience mental health and substance abuse challenges. Peer wellness specialists receive training focused specifically on reducing the levels of co-morbidity and shortened lifespan that are endemic among persons with behavioral health issues, and be active participants on primary care health teams.
Personal Health Navigator means an individual who provides information, assistance, tools and support to enable a patient to make the best health care decisions in the person’s particular circumstances and in light of the patient’s needs, lifestyle, combination of conditions and desired outcomes.
Doulas are certified professionals who provide personal, non-medical support to women and families throughout a woman’s pregnancy, childbirth and postpartum experience. The doula’s role is to help women have a safe, memorable and empowering birthing experience. Because doulas traditionally come from the communities they serve and have an intimate knowledge of the culture, they are uniquely positioned among the health care workforces to improve birth outcomes.
(Source: The material for this framework comes from the Oregon Health Authority’s report, The Role of Non-Traditional Health Workers in Oregon’s Health Care System, and the Oregon Health Authority House Bill 3331 Implementation Committee.)
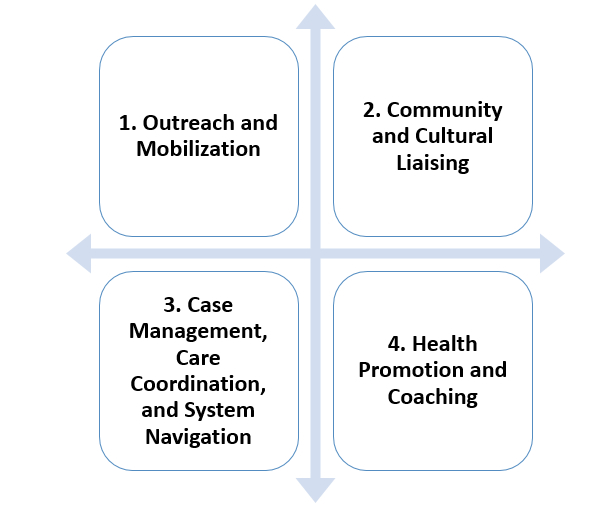
Roles of Non-Traditional Health Workers in the Health Care System
- Outreach and Mobilization: To support individuals, their identified families, and community members to gain the information and skills needed to effectively engage in healthy behaviors and in the health systems that support them.
- Community and Cultural Liaising: To identify and effectively bridge cultural, linguistic, geographic and structural differences which prevent or limit individuals’ ability to access health care or adopt health promoting or harm reducing behaviors.
- Case Management, Care Coordination, and System Navigation: To meet an individual’s holistic health needs through available resources in a timely and efficient manner, which may include recognizing and promoting system-level changes needed to meet individual and community needs. To assure the provision of culturally and linguistically appropriate services. To reduce duplicative, damaging or unnecessarily costly interventions that occur through lack of coordination.
- Health Promotion and Coaching: To assist individuals and their identified families in making desired behavioral changes and adopt behaviors that are sustainable, mutually acceptable, promote positive health outcomes, and are understood by families and community contacts. To identify and enhance individual, family, community, and social norms and strengths, as well as barriers to health and healthy behaviors.
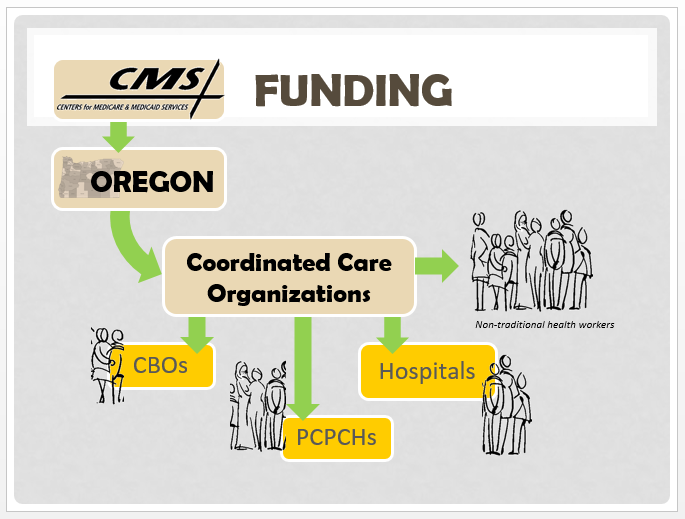
Non-Traditional Health Worker Funding Streams
Oregon has worked with the Centers for Medicare and Medicaid to obtain approval to pay non-traditional health workers with Medicaid dollars. The Oregon Health Authority has also created a structure and expectations that Oregon’s Medicaid health plans, the Coordinated Care Organizations, support the deployment of these workers in Community-Based Organizations (CBOs), Patient Centered Primary Care Homes (PCPCHs), and Hospitals.