It Begins with You
Self Management SupportSelf Management Support
Self-management support is the help given to people with chronic conditions that enables them to manage their conditions on a day-to-day basis. The Agency for Healthcare Research and Quality says it is important that the system of care supports the patient in their efforts to achieve improved health. However the patient cannot be expected to do this in a vacuum. Instead, the health care system needs to be designed in such a way that the physician, office environment, and health care organization all make changes to support patient self-management. Examples include:
- Providing empathic, patient-centered care.
- Involving the whole care team in planning, carrying out, and following up on a patient visit.
- Planning patient visits that focus on prevention and care management, as well as acute care.
- Involving the patient in goal setting.
- Providing tailored education and skills training that is culturally and linguistically appropriate.
- Making referrals to community-based resources, such as programs that help patients quit smoking or follow an exercise plan.
- Regular follow-up contact with patients via e-mail, phone, text messaging, and mailings to support them in efforts to maintain healthy behaviors.
The Oregon Health Authority succinctly describes taking control through self-management as:
- Working with your doctor as your healthcare partner
- Getting support from family and friends
- Knowing how to work through problems such as pain, fatigue, or depression
- Learning how to be active and eat well
- Understanding how to use medications correctly

The best thing a provider can do for their patients with chronic disease is to let them take charge of their own health (Funnell, 2000). Health care professionals tend to take credit for their patients’ successes, but when the patient isn’t doing well they say that person is noncompliant. In fact, the patient has more control of the outcome than the providers, even when they are successful. Patients need to be active and informed, and it is the provider’s role to encourage them to set self-management goals as they work toward self improvement. Funnell (2000) makes the following points:
The following diagram compares how a doctor might respond to a patient with a chronic disease in the old paradigm and provides an alternative in the new one.
- The old models of care where doctors tell patients what to do and try to motivate them to change don’t work.
- Because patients make decisions every day related to their health, they must be active, informed participants in the health care process.
- Physicians can support patients by encouraging them to set self-management goals that lead them toward greater health.
Source: Funnell MM (2000, March). Helping patients take charge of their chronic illnesses. Family Practice Management, v.7(3): 47-51.
Stanford Chronic Disease Self-Management Program
Stanford Medicine’s Chronic Disease Self-Management Program (CDSMP), is a six-week educational program for people with chronic conditions (e.g. arthritis, diabetes, lung and heart disease). Subjects covered include: 1) techniques to deal with problems such as frustration, fatigue, pain and isolation; 2) appropriate exercise for maintaining and improving strength, flexibility, and endurance; 3) appropriate use of medications; 4) communicating effectively with family, friends, and health professionals; 5) nutrition; 6) decision making; and 7) how to evaluate new treatments. The CDSMP workshops are provided in community settings such as senior centers, churches, libraries, and hospitals.
In an evaluation of the project, researchers found that subjects who took the CDSMP program, when compared to those who did not, reported better general health and less fatigue. They demonstrated significant improvements in exercise and communication with physicians, and they spent fewer days in the hospital. These patients had lower costs than those who did not participate in the program.
The American Institute for Research
The American Institute for Research developed a roadmap for practice and research to increase patient and family engagement in healthcare. Their vision is for the healthcare delivery system to meaningfully engage patients and families in every aspect of their health and healthcare. Ultimately the goal is for better patient experiences of care, better population health, and lower costs. The eight strategies for change are shown in the diagram below, and include topics such as patient and family preparation, clinician leadership preparation, and care and system redesign.

Source: The American Institute of Research’s Roadmap for Patient and Family Engagement in Healthcare
AIR proposes five actions that different constituencies can take to support patients and patient self-management. Examples of five things patients and clinicians can do are shown below. Additional information about actions other groups can take are documented on the Roadmap website.
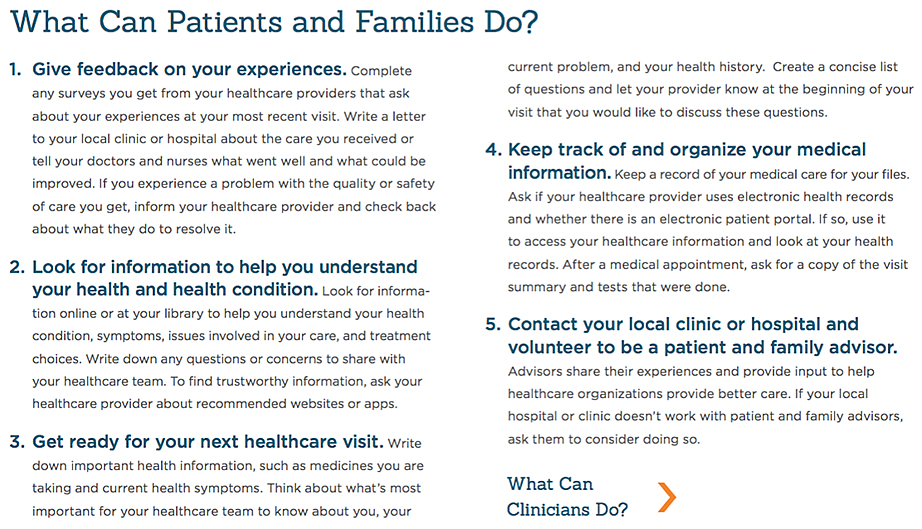
Source: The American Institute of Research’s Roadmap for Patient and Family Engagement in Healthcare
Josiah Macy Jr. Foundation
A conference held by the Josiah Macy Jr. Foundation in April 2014 called, “Partnering with Patients, Families, and Communities: An Urgent Imperative for Health,” brought together patients, advocacy organizations, health educators, and health care leaders to recommend how to make provider education and health care practices more responsive to patients and their families.
Innovative recommendations captured in a conference report identified a number of ways to enhance partnerships. One recommendation is to change how providers, students, patients, and family members are educated about health care and patient engagement. On this topic, participants made the following suggestions:
- Provide educational content that helps professionals learn to partner with patients, families, and communities.
- Include student participation in clinical practice in inpatient and outpatient settings to prepare them to incorporate patient and family engagement in their practice.
- Encourage patients and family members to co-educate students and other health care providers about their experiences, health status, and treatment.
- Change health care organizations’ practices and education to help personnel create a new vision and mission that incorporates patients, families, and members of the community as partners.
- Develop new skills and support mechanisms to create sustainable change.
- Institute regulatory and health care payment reform to support and sustain these changes in every payment delivery model.
There are numerous other suggestions worth investigating in the conference recommendations report.

